
- Shop
- Learn
-
-
- Buy The Sunflower Now
Feel the difference
Get Started with JustLight
Sunflower is the most advanced light therapy available today.

-
- Collaborate
- Blog
- Quiz
- My Account
Free Shipping in the 48 States!
A lack of understanding about the science behind Photobiomodulation therapy can leave consumers vulnerable to misleading marketing and create communication barriers between patients and medical professionals.
Buy Sunflower TodayPhotobiomodulation therapy (PBMT), commonly referred to as “red light therapy,” has gained significant traction in both the medical community and consumer markets over the past few decades. This non-invasive treatment, which uses specific wavelengths of light to penetrate the skin and tissues, has been validated through extensive research and is recognized by the FDA for its potential benefits across a wide range of health conditions. Today, red light therapy is a billion-dollar industry, with at-home light therapy devices becoming increasingly popular (GVR, 2023). Despite its growing popularity, there are many misconceptions surrounding red light therapy. A lack of understanding about the science behind PBMT can leave consumers vulnerable to misleading marketing and create communication barriers between patients and medical professionals.
To better understand current consumer knowledge of PBMT, we conducted a survey of 31 volunteers with varying levels of exposure to red light therapy. The goal was to assess their understanding of this therapeutic treatment and identify areas where education is needed. This article will discuss the survey results, clarify some common misconceptions about red light therapy, and explore the potential benefits of this treatment for various health conditions.
Our survey included 31 unique volunteers, most of whom were not existing customers of JustLight and had not previously engaged with our brand. This was done to minimize bias and ensure that the responses reflected a broad range of experiences with PBMT. Participants were asked to complete a 13-question survey that included questions about their past experiences with various PBMT services and technologies, as well as 10 True/False questions about PBMT. The survey also collected demographic information, such as age range and gender. After completing the survey, participants were directed to a blog post on our website that discussed each survey point in depth.
The demographic breakdown of our survey participants was as follows:
Of the 31 participants, 66% had some prior knowledge of PBMT, with 60% of these individuals being female.
The average score on the True/False section of the survey was 49.67% (SD = 28.9%), indicating a general lack of understanding of PBMT among the participants. Below are the top two questions that were answered correctly:
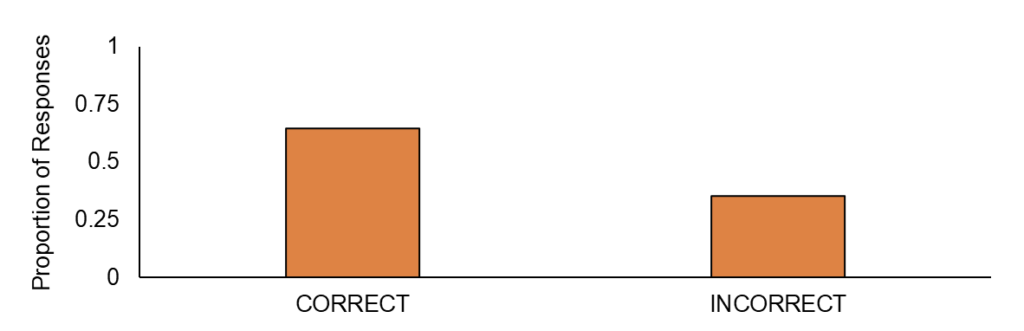
When asked whether different factors such as the type of light and dose of light-matter in red light therapy, 70.9% of respondents answered correctly, indicating that they understood that not all light is equal in effectiveness. This is promising, as the efficacy of photobiomodulation therapy largely depends on specific wavelengths of light, such as low-level wavelengths like red and near-infrared light, and their correct dosing. However, while participants seemed aware that these nuances exist, it is unclear if they fully understand how these factors influence treatment outcomes.
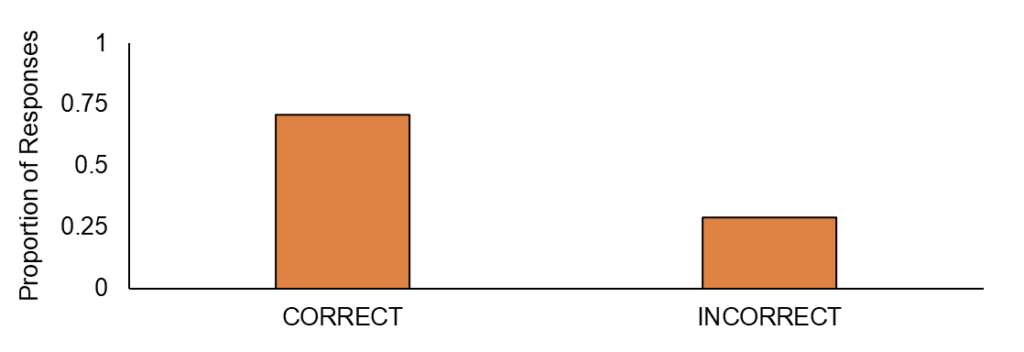
Eye safety is a critical aspect of using light therapy devices, and 64.5% of respondents correctly identified the importance of protecting their eyes during treatment. The FDA recommends that all manufacturers of light therapy devices include disclaimers about eye protection (FDA-2022-D-3116, 2023). Bright LEDs can cause temporary discomfort and visual aftereffects, such as making colors appear more blue or green (Thompson & Burr, 2009). Interestingly, while PBMT can benefit eye health when used to heal retinal injuries (Eells et al., 2016), it is essential for users to take precautions when using these devices for non-ophthalmic concerns.
Below are the top two questions that were most frequently answered incorrectly, highlighting common misconceptions about red light therapy:
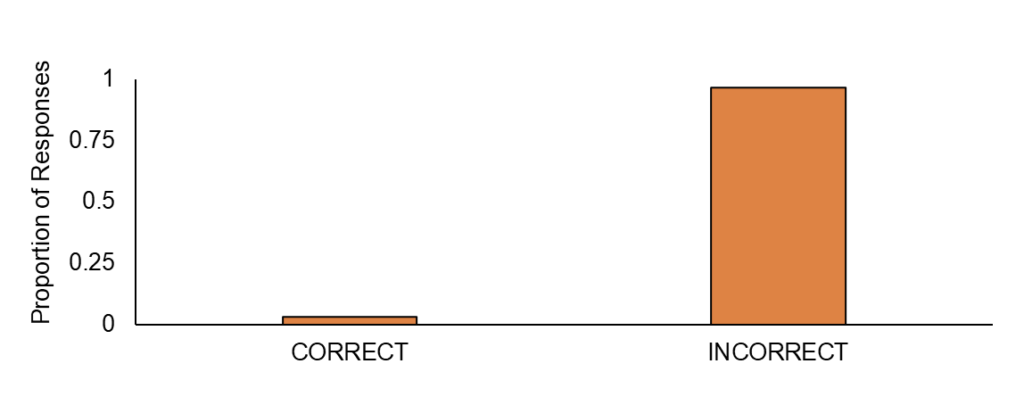
A surprising 96.7% of participants incorrectly believed that red light therapy could be effective through clothing. In reality, infrared light is readily absorbed by fabrics, and red light can be reflected or absorbed depending on the color of the clothing. This misconception can lead to ineffective treatments, as the light cannot penetrate the skin and reach the target cells if blocked by clothing. For effective treatment, it is crucial to use PBMT on clean, bare skin. Additionally, skincare products, such as makeup, should be avoided during treatment because their pigments can react with the light, further diminishing its effectiveness.
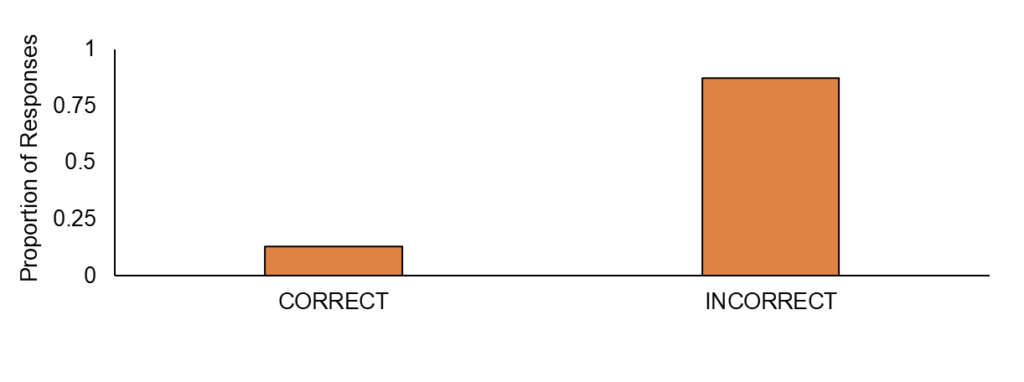
Approximately 32.2% of respondents incorrectly believed that full-body red light therapy provides the same benefits as targeted therapy. However, there is no robust data directly comparing the efficacy of full-body and targeted PBMT. Clinical studies have predominantly focused on localized treatments, revealing that optimal dosing parameters differ between various areas and tissue types (Zein et al., 2018). Full-body PBMT, often marketed as a convenient, all-encompassing solution, lacks the rigorous testing that localized treatments have undergone. As a result, consumers may be misled into purchasing expensive full-body devices without understanding the limitations and unproven efficacy of these products.
Our survey highlights a critical need for better consumer education on the science and practical use of red light therapy. While there is some awareness of the importance of light type and dose, many consumers still hold misconceptions that could lead to ineffective or misused treatments. For instance, the belief that red light therapy can be effective through clothing or that full-body treatments are equally beneficial as targeted therapies can result in disappointing outcomes.
Photobiomodulation therapy, which includes red light therapy, is based on the principle that specific wavelengths of light can penetrate the skin and stimulate cellular processes. These light therapy devices, particularly those using low-wavelength red and near-infrared light, have been shown to enhance cellular functions, such as ATP production, which is vital for energy levels and cellular activity. These processes contribute to a range of therapeutic benefits, including collagen production, wound healing, and improved skin health.
Red light therapy offers numerous potential benefits, including:
Given the variety of light therapy devices on the market, it is essential for consumers to choose a device that meets their specific needs. Factors to consider include the type of light used, the wavelengths, the power density, and the intended use (e.g., skin rejuvenation, pain relief, hair regrowth). It is also important to consider the safety features of the device, such as protective eyewear and FDA approval, to ensure safe and effective treatment.
Overall, our survey underscores the need for improved education on photobiomodulation therapy to ensure that consumers can make informed decisions about at-home use. While many consumers understand the importance of safety and the nuances of choosing the right type and dose of light, there is still a lack of clarity on what makes a reliable PBM device and how to use it effectively.
For researchers, doctors, and companies involved in photobiomodulation therapy, it is crucial to focus on educating consumers about the science behind red light therapy. This includes providing clear instructions on device usage, addressing common misconceptions, and sharing evidence-based information on the potential benefits and limitations of PBMT.
By enhancing consumer knowledge, we can improve patient satisfaction rates, optimize treatment outcomes, and bridge the gap between patients and medical professionals when discussing red light therapy as a viable treatment option.
By staying informed and understanding the nuances of red light therapy, consumers can take full advantage of this effective treatment option for a variety of health conditions, while ensuring safety and efficacy in their at-home use.
Photobiomodulation Therapy (PBMT) is the scientific term for what is commonly known as red light therapy. PBMT involves using specific wavelengths of light, including red and near-infrared light, to penetrate the skin and tissues, stimulating cellular processes that promote healing, reduce inflammation, and improve skin health. While PBMT is the broader scientific concept, red light therapy specifically refers to using red wavelengths in the visible spectrum for therapeutic purposes.
Yes, red light therapy is generally safe for at-home use, especially when using FDA-recognized light therapy devices. These devices are designed to deliver therapeutic benefits with minimal risk of side effects. However, it is essential to follow the manufacturer’s instructions carefully, use protective eyewear, and ensure the skin is clean and free from any lotions or makeup during treatment to maximize safety and effectiveness.
Yes, red light therapy has a broad range of potential benefits beyond skin health. It is used for wound healing, pain relief, muscle recovery, joint pain, hair growth, and even improving cognitive functions. Red light therapy’s ability to stimulate cellular activity and reduce inflammation makes it a versatile treatment option for various health conditions.
No, red light therapy is not effective through clothing or makeup. Fabrics, especially thick or dark-colored ones, absorb or reflect the light, preventing it from reaching the skin and target cells. For optimal results, red light therapy should be administered on clean, bare skin without any barriers like clothing, makeup, or lotions that could impede light absorption.
When selecting a light therapy device, consider factors such as the type of light used (e.g., red light, near-infrared light), the wavelength range, the power density, and the device’s intended use (e.g., skin rejuvenation, pain relief). It’s also important to choose a device that is FDA-recognized and includes safety features like protective eyewear. For personalized treatment plans, it’s advisable to consult with a healthcare professional before starting red light therapy.